Fertility Treatment Methods: Modern Options for Growing Your Family
Personalised care, advanced diagnostics, and proven technologies at Kinderwunschzentrum Dresden
For many, having a child is one of life’s greatest wishes. When natural conception doesn’t occur, assisted reproduction offers a range of effective options. One of the core pillars is fertility treatment – encompassing various medical techniques to support people on their journey to parenthood.
Modern reproductive medicine now provides tailored solutions for couples and individuals, regardless of their medical history or family structure. Whether due to hormonal imbalances, low sperm quality, endometriosis or unexplained infertility – we take a holistic, compassionate and evidence-based approach to find the best path forward.
Below, we explain how fertility treatment works, which methods are available, and what steps are involved.
Step-by-Step: How Fertility Treatment Begins
- Initial Consultation
Your journey starts with a detailed conversation with our fertility team. We listen to your story, medical history and treatment goals. Emotional wellbeing is also a key part of our approach. - Diagnostic Testing
To determine the cause of infertility, we offer a wide range of diagnostics:- Hormone level checks
- Semen analysis
- Ultrasound scans
- Cycle monitoring
- Genetic or immunological testing, where needed
Only by understanding the root cause can we design a treatment plan that fits.
- Choosing the Right Method
Following diagnosis, we recommend the most suitable fertility treatment. This may range from mild hormonal support to IVF or ICSI, depending on your situation. All options are explained clearly and transparently. - Financial Planning
We help you understand the costs involved, and advise on potential insurance reimbursements or financial assistance options.
Overview of Fertility Treatment Methods
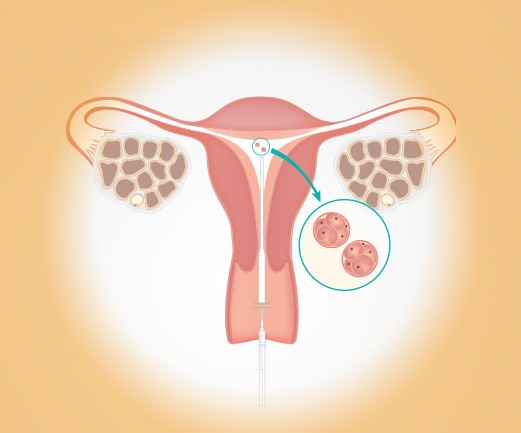
In Vitro Fertilisation (IVF)
Eggs are retrieved and fertilised with sperm in the lab. After fertilisation, one embryo is transferred to the uterus.
Recommended for:
- Blocked fallopian tubes
- Endometriosis
- Unexplained infertility
- After tubal sterilisation
Benefits:
- Highly controllable
- Can be combined with additional laboratory measures
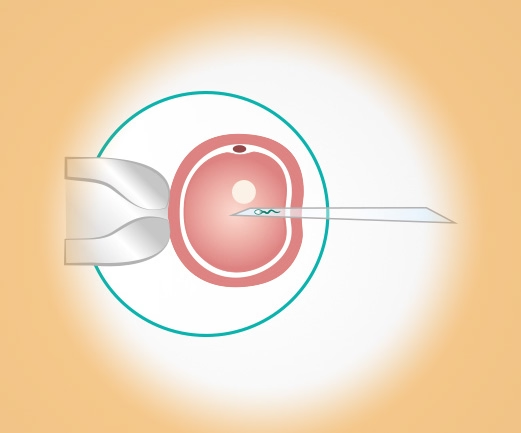
ICSI / PICSI
With ICSI, a single sperm is injected directly into an egg. PICSI is a refinement that selects the best sperm before injection.
Recommended for:
- Poor sperm quality
- IVF cycles with failed fertilisation
- CatSper deficiency (functional sperm issue)
Benefits:
- Enables conception despite severe male infertility
- High success rates when applied in the appropriate setting
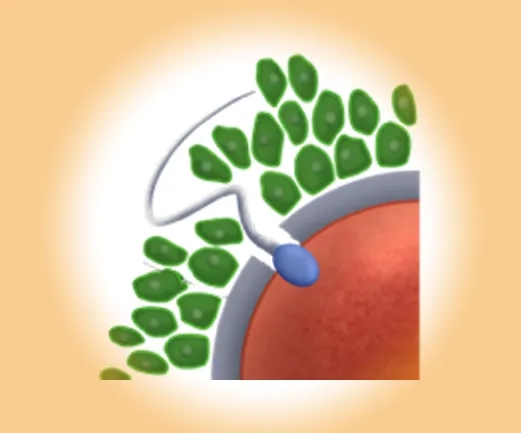
Intrauterine Insemination (IUI)
Prepared sperm are placed directly into the uterus near ovulation. Often combined with mild hormonal stimulation.
Recommended for:
- Mild male factor infertility
- Ovulation disorders
- Unexplained infertility
Benefits:
- Non-invasive
- Lower cost
Sperm Donation
When own sperm is not usable, donor sperm from certified banks may be used. Suitable for single women, lesbian couples, or male infertility.
Benefits:
- Legally regulated
- Identity of donor available to child at age 16
TESE (Testicular Sperm Extraction)
Surgical retrieval of sperm directly from testicular tissue for use in ICSI.
Recommended for:
- Azoospermia (no sperm in ejaculate)
- After vasectomy
Benefits:
- Outpatient procedure
- Sperm can be frozen for future use
Supportive Lab Measures for Higher Success Rates
Assisted Hatching
A laser thins the embryo’s outer shell to help implantation.
Recommended for: Women over 35, thick zona pellucida, repeated IVF failures
EmbryoGlue
A hyaluronic acid-rich medium used during embryo transfer to improve adhesion.
Recommended for: Implantation disorders, multiple failed attempts
Blastocyst Transfer
Embryos are transferred at day 5 when more development information is available.
Benefits: Better implantation potential, single embryo transfer reduces risk of multiples
Zymot Chamber
Selects high-quality sperm without centrifugation. Improves outcomes in IVF/ICSI.
Benefits: DNA-safe selection, better fertilisation and pregnancy rates
Time-Lapse Incubator
Continuous monitoring without removing embryos from the incubator.
Benefits: Improved embryo selection, non-invasive
Cryopreservation: Preserving Fertility
Embryo Cryotransfer
Embryos are frozen and transferred in a future cycle.
Benefits: No repeat stimulation, equally high success rates
Sperm Freezing
Used before chemotherapy or surgery, or in case of impaired sperm production.
Social Freezing
Unfertilized Eggs are frozen for future use to preserve fertility.
Recommended for: Women under 35, long-term planning
Medical Freezing
Preserves fertility before medical treatments (e.g. cancer therapies).
Benefits: Fertility protection during major health challenges
Supporting Body & Mind
Acupuncture
May enhance blood flow to the uterus and reduce stress.
Couples & Sexual Counselling
Address emotional strain, intimacy issues, and communication within relationships.
Peer Support Group
Connect with others experiencing infertility in a guided, confidential setting.
Success Rates & Risks
Success Chances
Success depends on age, diagnosis and treatment type. In Germany, pregnancy rates per embryo transfer are around 37% (DIR 2023). After 4 cycles, up to 70% of women achieve pregnancy.
Age matters:
- <35 years: up to 40%
- 35-39 years: 30–40%
- 40+ years: 10–20%
Risks
- Multiple pregnancies: Mitigated through single embryo transfer
- Ovarian Hyperstimulation (OHSS): Monitored with personalised protocols
Let’s Talk
Want to find out which method is best for you?
Book a personal video consultation with Kinderwunschzentrum Dresden today.
Dresden Fertility Center
in the Wöhrl Plaza
Prager Str. 8a
01069 Dresden
Phone +49 351 501 400-0
Fax +49 351 501 400-28
Email:
Instagram Arrange your first appointment NEW: Video consultation! Downloads Impressions
Cryobank in the Kinderwunschzentrum Dresden
Prager Str. 8a
01069 Dresden
Tel. +49 351 50140019
E-Mail:
| Office hours | |
|---|---|
| Mon., Wed., Thu. | 08.00 – 19.00 Hrs |
| Tue. | 08.00 – 13.00 Hrs and 14.30 – 19.00 Hrs |
| Fri. | 08.00 – 14.00 Hrs |
Availability by telephone |
|
| Mon., Wed. | 08.00 – 13.00 Hrs and 14.30 – 18.00 Hrs |
| Tue., Thu., Fri. | 08.00 – 13.00 Hrs |
Blood sampling |
|
| Mon. - Thu. | 08.00 – 17.30 Hrs |
| Fri. | 08.00 – 13.30 Hrs |
On Tuesdays the clinic is closed from 13.00 to 14.30 Hrs! |
|
Service at the Fertility Center Dresden

To the planned child